Detail
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
This can be advantageous when weaning patients from mechanical ventilation. The dead space takes no part in gas exchange and adds to the work of breathing. Reducing this can help patients with critical respiratory reserves get off a ventilator.
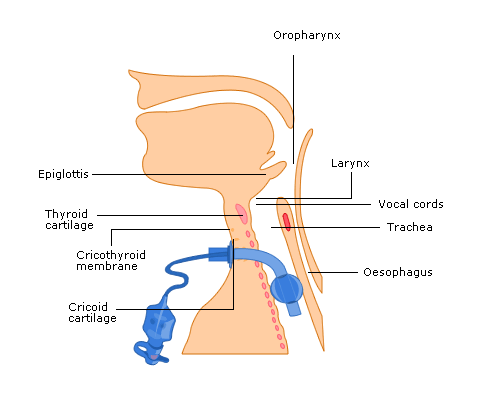
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
-
The natural warming, humidification and filtering of air that
usually takes place in the upper airway is lost
- Fig 1 is a video describing humidification
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
This is one of the biggest dangers with a tracheostomy or laryngectomy. Secretions will become thick and dried and can easily obstruct a stoma or tube. This situation is made worse if there are copious secretions – often the case with these patients.
Learn how to keep the respiratory gases humidified in the nursing care section.
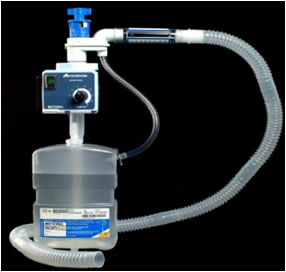
Humidifier
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
-
The natural warming, humidification and
filtering of air that usually takes place in the upper airway is
lost
- Fig 1 is a video describing humidification
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
-
The patient's ability to speak is removed
- Fig 2 is a video of the patient's experience of losing their voice
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
This is a big problem for the patient and can lead to distress and anxiety.
Sometimes, we can use aids like speaking valves to help patients vocalise, but attentive and nursing staff are probably the most valuable source of help. Communication boards can be useful too.

Communicator
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
-
The
patient's ability to speak is removed
- Fig 2 is a video of the patient's experience of losing their voice
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
Most people with a new tracheostomy will have a naso-gastric or similar feeding regimen established.
The cuff of the tracheostomy or the tube itself interferes with the swallowing mechanics of the larynx. These muscles can waste if not used (during prolonged ventilation) and require careful rehabilitation and assessment. The Speech and Language Therapist (SALT) is an essential member of the multi-disciplinary team.
Click here to watch a nasendoscopic video of a SALT swallowing assessment.
Note the aspiration of fluid through the vocal cords and that the patient does not cough.
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
This can reduce appetite and general wellbeing of the patient. Patient’s report this as a significant problem which can be easy to overlook when managing their ‘medical’ problems.
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image
This is an important factor as it can have a major psychological impact. If possible the patient should have careful preoperative explanation. If this is not possible the patient must receive explanation and support postoperatively.
Inform the patient that scarring will be minimal when the tracheostomy is removed and the stoma has healed and, that speech will return (as long as the vocal cords remain intact). On average the stoma will close and heal within 4-6 weeks. However this may vary from patient to patient depending on factors affecting wound healing.
Physiological changes with a tracheostomy:
- The upper airway anatomical dead space can be reduced by up to 50%
- The natural warming, humidification and filtering of air that usually takes place in the upper airway is lost
- The patient's ability to speak is removed
- The ability to swallow is adversely affected
- Sense of taste and smell can be lost
- Altered body image